HCR Patient Education
Medical jargon and recommendations for treatments or tests can be very intimidating. The Hinsdale Center for Reproduction has put together this education page to help you understand procedures that you may have discussed with the HCR staff. You will find basic information about some diagnoses and testing procedures.
You are not Alone. About one out of every six couples who desire children has an infertility problem. In these pages, The Hinsdale Center for Reproduction hopes to answer some of the questions our patients ask. If you need additional information, please feel free to call us at 630-856-3535.
Treatment of Infertility
In the mid 1990's, the practice of infertility changed dramatically, driven largely by the medical insurance industry. In the state of Illinois, legislation was championed in Springfield to include infertility services in the standard Health Care insurance policy. Infertility care became a "covered" condition, and large IVF centers developed to accommodate the increased number of patients. These large centers concentrate on IVF, and most are very successful at achieving pregnancies with patients who fall within "normal" parameters.
However, if an individual patient has a surgical problem contributing to their infertility, they need to be referred to a physician with the surgical skills to correct that problem. Dr. Hickey's training was in programs with strong emphasis on surgery, specifically Georgetown University Medical Center and the University of Southern California. Twenty-five years ago, Dr. Hickey trained with many nationally known physicians - many of whom actually invented the standard procedures commonly employed today. These techniques have undergone constant improvement and "tweaking" as new materials and instruments are developed.
Hysteroscopic Non-Invasive Surgery
Sometimes irregularities in a woman’s body may not allow her to get pregnant or maintain a pregnancy. No amount of IVF can solve the problem. Dr. Hickey has found that by using a hysteroscope for viewing and operating, he can correct problems standing in the way of pregnancy in a non-invasive manner.
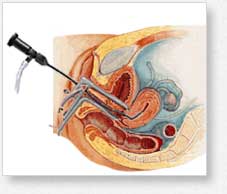 Unlike laparoendoscopic surgery, that requires making an incision, hysteroscopic surgery enters through natural body openings. The procedure is painless and is done under general anesthetic.
Unlike laparoendoscopic surgery, that requires making an incision, hysteroscopic surgery enters through natural body openings. The procedure is painless and is done under general anesthetic.
The hysteroscope is basically a long, flexible telescope connected to a light source. The tip is only 3 mm wide and passes easily through the dilated cervix. This makes the procedure quick and easy. Most women are back to their full routines the next day.
Dr. Hickey attaches a camera to the hysteroscope and watches the progress on a television screen. Paired with a morcellator attachment, the hysteroscope gives Dr. Hickey not only the ability to see but to remove and suction out tissue fragments. Dr. Hickey uses the instrument to reshape the uterus, clear adhesions and blockages.
Dr. Hickey trained at USC with the doctor who developed this procedure. Dr. Hickey is one of only a handful of U.S. surgeons offering Hysteroscopy Procedures.
Pre-Implantation Genetic Diagnosis (PGD) and
Pre-Implantation Genetic Screening (PGS)
Pre-Implantation Genetic Diagnosis (PGD) refers to the ability to remove cells from a developing egg or embryo and analyze them for the presence of one of several types of genetic abnormality. Using techniques largely developed in the Human Genome Project, families affected by a potentially unlimited number of inherited diseases can reduce the risk that their children will suffer that disorder.
When we do PGD, we know ahead of time that one or both of the parents has a particular genetic mutation or chromosomal rearrangement that the embryo is at risk for inheriting. So the purpose of undergoing PGD is to rule out which embryos are affected and only use the unaffected embryos. This will greatly minimize the chance of having a pregnancy that is affected with an abnormality. Because of the time needed for such sophisticated analysis, embryos tested with PGD will need to be frozen and transferred back to the patient in a subsequent Frozen Embryo Transfer (FET) cycle.
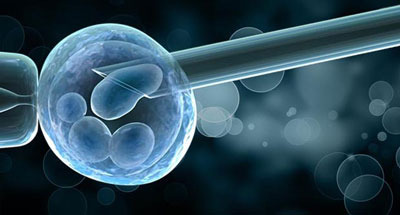 PGD and PGS can be performed either from a day 3 embryo biopsy, when a blastcyst is removed from an 8 cell embryo, or from a trophectoderm biopsy obtained from a day 5 or 6 embryo called a blastocyst.
PGD and PGS can be performed either from a day 3 embryo biopsy, when a blastcyst is removed from an 8 cell embryo, or from a trophectoderm biopsy obtained from a day 5 or 6 embryo called a blastocyst.
We prefer to do PGD and PGS on day 5 embryos. There is more genetic material to work with, and the biopsy is less likely to disrupt the embryo’s progress. The cells are tested by a process called Array Comparative Genomic Hybridization (a-CGH)

We’re here to help you.
For more information, call The Hinsdale Center for Reproduction: 630-856-3535